Introducing Nutrition Management 2.0
A comprehensive, guideline-driven approach that unites nutritional assessments with technological innovation to prevent feeding-related complications in critical care.

Key Principles
Hospital nutrition, particularly in the ICU, where accurate care is often a matter of life and death, has not been at the forefront of clinical education. However, research has shown evidence of the underlying challenges concerning nutrition-related in-hospital complications. We are advancing intensive care nutrition therapy by focusing on greater precision, personalization, and safety.
Redefining Scoring Systems
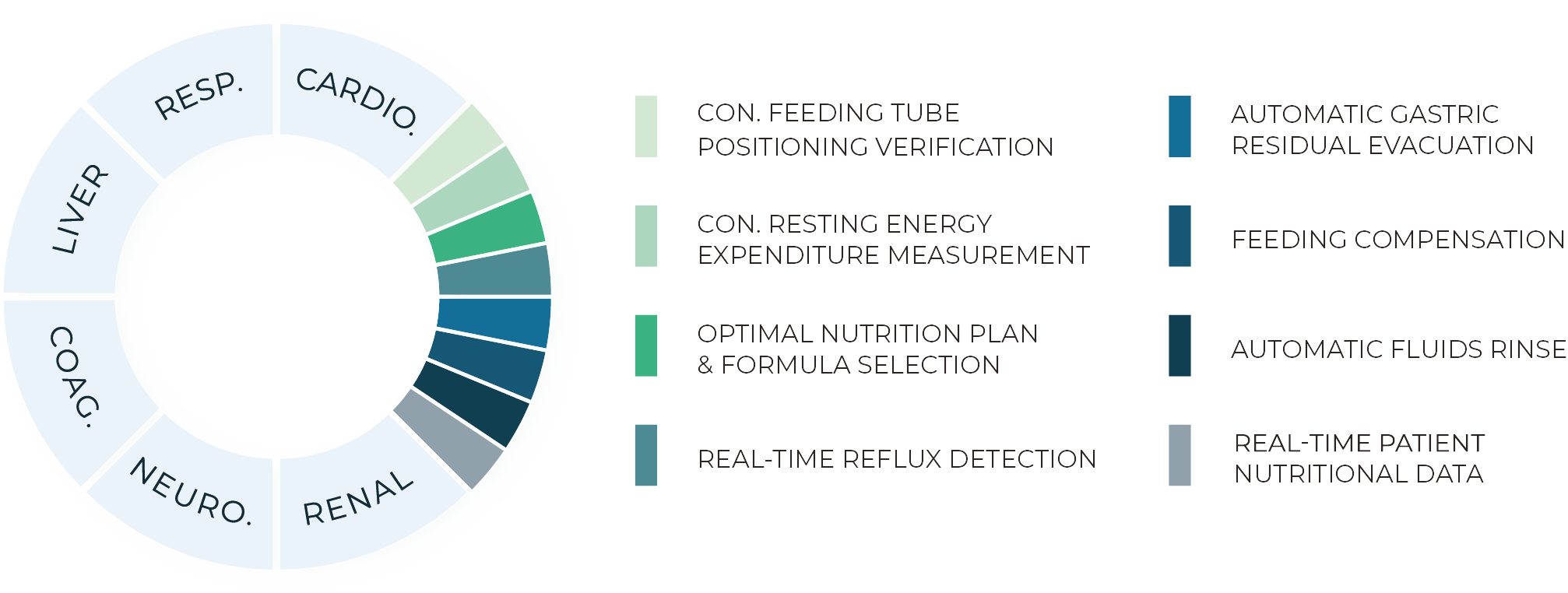
Current scoring systems do not take into account feeding-related elements which actively impact critically ill patients.
Creating a New Paradigm
Optimal nutrition therapy is a key component of critical care. Yet ICU patients are routinely subjected to the risks of malnutrition, tube malposition and pneumonia. Prof. Pierre Singer explains how Nutrition Management 2.0 is changing the traditional approach and provides a new and comprehensive nutritional therapy practice.


 Global Site
Global Site